Personal Stratified Follow-Up And Supported Self-Management
Personal Stratified Follow-Up
 Adapted from a long term conditions model, personal stratified follow-up is an approach to profiling patients following treatment for cancer that is based on their clinical and individual needs. It is applied to all patients whether they have been treated with curative or palliative intent and provides a more tailored approach to aftercare services, improved information and education and care closer to home where appropriate.
Adapted from a long term conditions model, personal stratified follow-up is an approach to profiling patients following treatment for cancer that is based on their clinical and individual needs. It is applied to all patients whether they have been treated with curative or palliative intent and provides a more tailored approach to aftercare services, improved information and education and care closer to home where appropriate.
There is no 'one size fits all' and many patients welcome not having to return to hospital for their appointments.
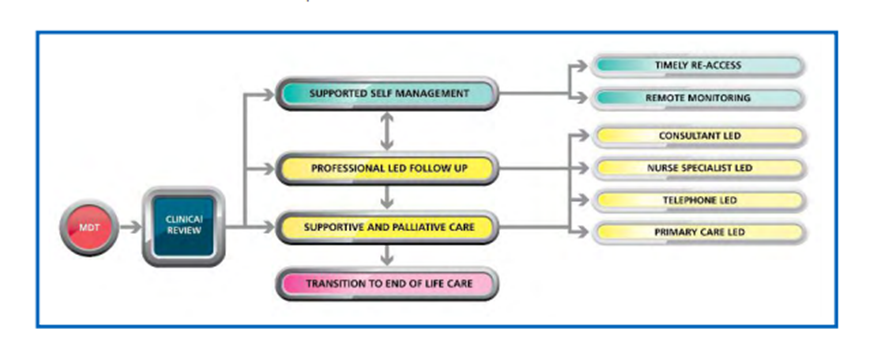
Pathway choice is a joint decision between the individual and the clinician, dependent on level of patient risk. It is essential to have personalised stratification guidelines and pathways in place, for patient safety. Patients can be stratified into the following pathways of professional follow-up (consultant and nurse), supported self-management and supportive and palliative care.
The supported self-management pathway is dependent upon the presence of other key components of the pathway. These include:
- digital remote monitoring system to manage ongoing surveillance tests
- effective assessment that identifies and addresses outstanding needs and ensures the patient has the knowledge and confidence to self-manage their condition and recovery, such as patient activation tools
- good communication between specialist and primary care teams
- a clinical pathway that allows rapid re-access to the specialist team if needed
The NHS Long Term Plan states that this stratified follow-up approach would be established in all trusts for breast cancer in 2019, for prostate and colorectal cancers in 2020 and for other cancers where clinically appropriate by 2023.
Personal stratified follow up and supported self management also form part of the Optimal Pathway Groups workstream, and the OPGs are instrumental in sharing good practice and standardising ways of working among specialties across West Yorkshire and Harrogate.
The OPGs take a whole pathway approach and some of the benefits for streamlining follow-up can be realised at the front end of the pathway, leaving more resource available to focus on newly diagnosed patients and more complex cases.
The Cancer Alliance was keen to engage with patients about what was important for them when looking at pathways for implementation. This report outlines the start of that engagement, summarising discussions with the Cancer Alliance community/patient panel in April 2020.
Learn more about the community/patient panel
Supported Self-Management
 Supported Self-Management Follow-Up (SSMFU) is a model whereby patients manage their own follow-up, with back-up from clinical teams as needed, in order to limit risk and ensure a satisfactory patient experience closer to home.
Supported Self-Management Follow-Up (SSMFU) is a model whereby patients manage their own follow-up, with back-up from clinical teams as needed, in order to limit risk and ensure a satisfactory patient experience closer to home.
Patients access workshops, education and relevant detailed information to ensure they are adequately prepared.
They are supported to enable recovery with a healthy lifestyle and preparation for all the potential consequences of cancer and their treatment.
There is a clear protocol for re-entry to the service if and when required. Routine follow-up investigations continue as before with robust tracking and standard clinical follow-up continuing for those not suitable for SSMFU.
Useful Information
Case Study: Supported Self-Management Patient Education Bursary Scheme
Click here to learn more about our supported self-management patient education bursary scheme for 2019/2020








